Electrocardiography (ECG or EKG) is a crucial diagnostic tool in the field of cardiology. It provides valuable insights into the electrical activity of the heart and can aid in the detection of various heart conditions. Among the many components of an ECG, the R-wave progression is a vital indicator. When misdiagnosed or misinterpreted, especially in the context of poor R-wave progression, the consequences can be significant. In this article, we will explore the importance of R-wave progression in ECG and the potential costs associated with its misdiagnosis.
Understanding R-Wave Progression
The Meyers Gluten Free describe, R-wave progression refers to the pattern of changes in the R-wave amplitude as one moves across the precordial (chest) leads in a standard 12-lead ECG. The R-wave typically starts small in lead V1 and becomes progressively larger in leads V2 to V6. This pattern is considered normal and indicates proper electrical conduction through the heart’s ventricles.
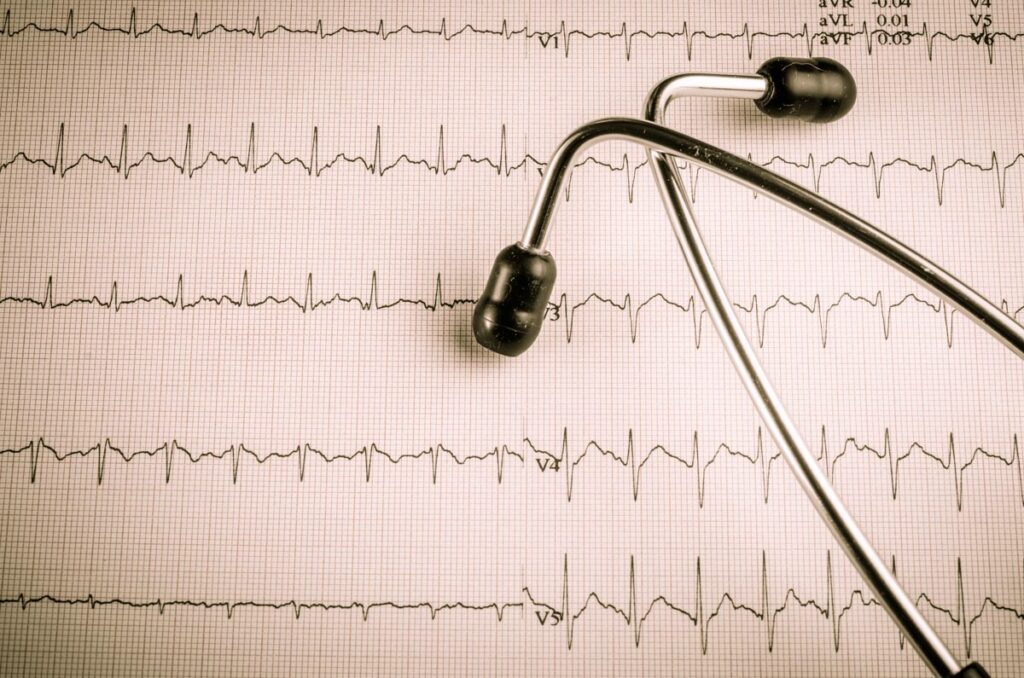
Significance of R-Wave Progression
Detecting Cardiac Abnormalities
Poor R-wave progression can be a sign of underlying cardiac abnormalities, such as myocardial infarction (heart attack), left ventricular hypertrophy (enlargement of the heart’s main pumping chamber), or conduction abnormalities. Detecting these conditions early is crucial for prompt treatment and better outcomes.
See also – Exploring Glaucoma Treatment: Is Glaucoma Surgery the First Choice?
Risk Assessment
Proper interpretation of R-wave progression helps assess a patient’s risk for cardiac events. Abnormal R-wave progression can indicate a higher risk, leading to more vigilant monitoring and preventive measures.
The Costs of Misdiagnosis
Misdiagnosis or misinterpretation of ECG findings, especially related to poor R-wave progression, can have various costs, including:
Delayed Treatment
If a patient’s ECG is misread, and poor R-wave progression is not identified, there can be a delay in the diagnosis and treatment of underlying cardiac conditions. Delayed treatment can lead to disease progression, complications, and poorer patient outcomes.
Unnecessary Procedures
On the flip side, a false positive diagnosis of poor R-wave progression can lead to unnecessary medical procedures, including angiography or cardiac catheterization. These procedures carry inherent risks and financial burdens.
Increased Healthcare Costs
Both delayed treatment and unnecessary procedures contribute to increased healthcare costs. Patients may incur expenses related to additional tests, hospitalizations, and medications.
Emotional Stress
Misdiagnosis can cause emotional stress and anxiety for patients and their families. The uncertainty and fear associated with a potentially serious cardiac condition can have a lasting impact on mental health.
Legal and Ethical Implications
In cases of severe misdiagnosis or negligence, there can be legal and ethical repercussions for healthcare providers. Malpractice claims can result in significant financial penalties and damage to a healthcare provider’s reputation.
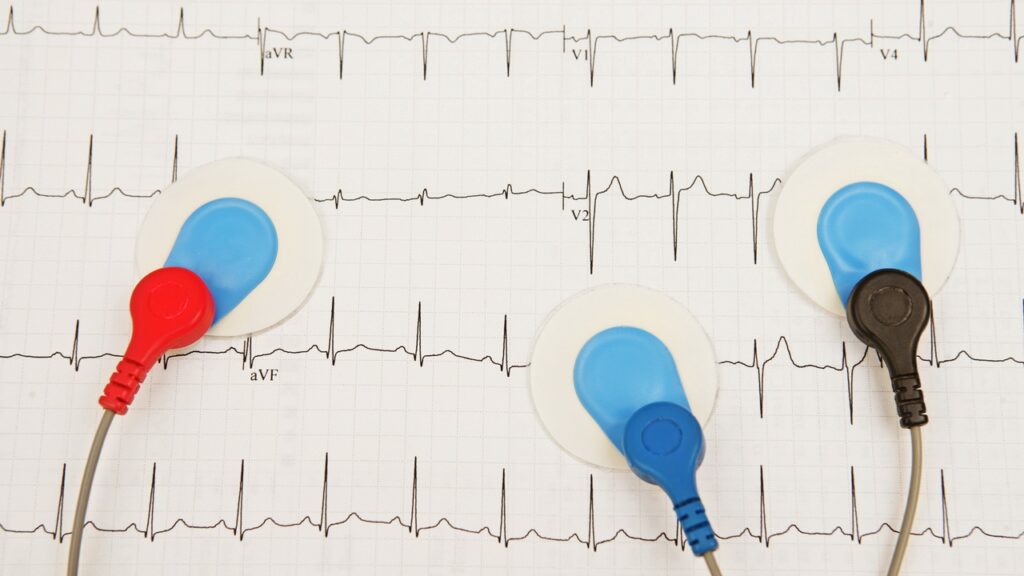
Preventing Misdiagnosis
To minimize the costs, both human and financial, associated with ECG misdiagnosis, healthcare providers should prioritize the following:
Education and Training
Continuous education and training for healthcare professionals, especially those involved in ECG interpretation, are essential. Staying up-to-date with the latest guidelines and diagnostic criteria is crucial.
Quality Assurance
Healthcare facilities should implement quality assurance programs that include regular audits of ECG interpretations. Peer review and feedback mechanisms can help identify and rectify interpretation errors.
Advanced Technology
Utilizing advanced ECG technology, including computer-assisted interpretation algorithms, can enhance accuracy and reduce the risk of human error.
Collaboration
Promoting interdisciplinary collaboration among healthcare providers, including cardiologists, nurses, and technicians, can lead to more accurate diagnoses and better patient care.
In conclusion, ECG misdiagnosis due to poor R-wave progression can have significant costs, both in terms of patient outcomes and healthcare resources. Recognizing the importance of proper ECG interpretation, investing in education and technology, and promoting a culture of collaboration and quality assurance are essential steps in mitigating these costs and ensuring the accurate diagnosis of cardiac conditions. Ultimately, the goal is to provide timely and effective care for patients, improving their overall quality of life.